Medical-Dental Integration
Treating the whole person requires breaking down silos between medical and dental care.
The Connection Between Oral Health and Overall Health
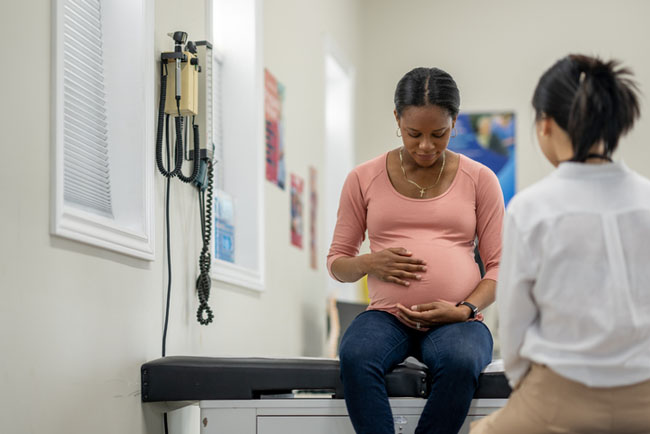
Oral health is inextricably connected to overall health. Dental disease can lead to high blood pressure, make it harder to manage diabetes, raise the risk of developing Alzheimer’s disease, and result in pregnancy complications. Good oral health practices and preventive dental care, on the other hand, can benefit overall health.
But despite the growing understanding of this relationship, oral health care often remains isolated from the rest of the health care system.
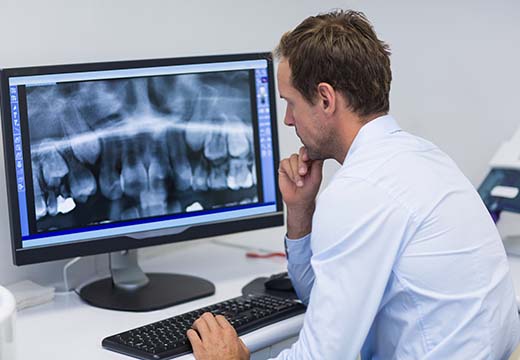
Medical-dental integration can help build that critical bridge between oral health and overall health. This approach to care integrates dental medicine into primary care and behavioral health, while also integrating services such as screenings for chronic diseases into dental care. It is an approach to care that encourages providers to come up with comprehensive care plans for the whole person.
Stats
2-3x
People with gum disease have 2 to 3 times the risk of having a heart attack, stroke, or severe cardiovascular event.
Learn more
22%
At least one preventive dental visit within three years reduced the likelihood of a ventilator-associated pneumonia (VAP) diagnosis by 22%.
Learn more
10
Having 10 years of chronic gum disease (periodontitis) was associated with a higher risk of developing Alzheimer’s disease.
Learn more
86%
Diabetes raises the risk of developing gum disease (periodontitis) by 86%.
Learn more
$520M
Medicaid spends $520 million annually on dental emergency department visits.
Learn more
27M
27 million people see a dentist but not a physician each year.
Learn more
The Value of Medical-Dental Integration
In addition to improving health outcomes, medical-dental integration can reduce costs.
Every year, Medicaid spends $520 million on dental emergency department visits, many of which could be avoided if symptoms were addressed before they became severe. Oral health problems make other conditions worse, leading to increased expenditures and negative outcomes in other areas of health care, as well.
An integrated approach can catch and manage problems earlier. For example, when patients visit their primary care provider, there’s an opportunity to assess oral health risk and reinforce at-home care messaging. This creates an access point for patients who might not otherwise seek dental care, particularly for the most vulnerable populations.
Recent Progress Toward Integration
Many community health programs and Federally Qualified Health Centers (FQHCs) are already working toward medical-dental integration. For example, CareQuest Institute’s MORE Care initiative engaged primary care practices across the country to integrate oral health competencies and capabilities into their offices while building patient-centered referral networks with local dental providers. These collaborative approaches educate patients about the connections between oral health and overall health, promoting prevention behaviors and strategies.
In addition, some dentists provide screenings for chronic diseases such as diabetes, high blood pressure, and cholesterol.
Care Coordination & Interoperability
In order to make medical-dental integration a reality, providers from across the system need tools to coordinate care. This includes ensuring that health information systems are interoperable — that is, that different devices and information systems can access, exchange, integrate, and use data in a coordinated manner.
All providers caring for a given patient must have access to the same information and be able to communicate seamlessly with one another. That coordination is critical to providing the right care in the right place at the right time. Interoperability in health care helps make that possible.
The oral health system is behind the medical system when it comes to sharing information electronically. One of the major restrictions for information exchange standards in dentistry is the limited use and slow adoption of electronic health records (EHRs) by the industry. In fact, it wasn’t until about 2017 that more than half of dentists utilized EHRs in practice. Dentistry is now in a position of playing catch-up and trying to integrate with the medical system.
Improving Coordination and Interoperability
CareQuest Institute is working with innovators and leading health care organizations — through initiatives such as MORE Care and COrHT — to identify emerging technologies that will advance care coordination.
Also, as part of the Dental Data Exchange Project, CareQuest Institute helped develop the first implementation guides to bridge the communication gap between primary care and oral health care.