Medicaid
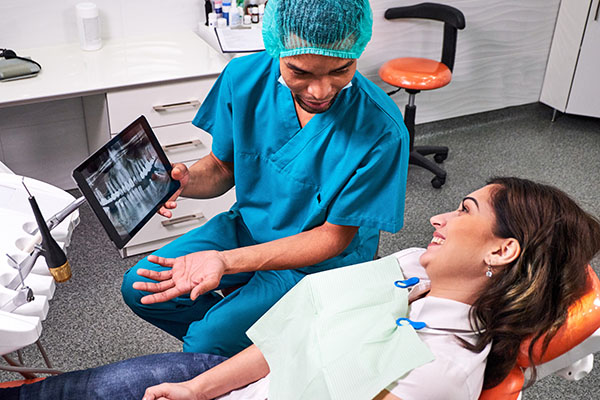
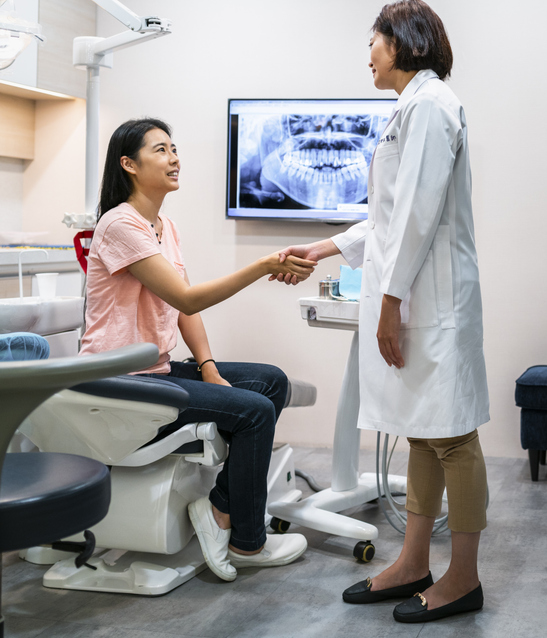
Adding oral health coverage for adults enrolled in Medicaid — which is optional for states — can save states money, reduce costly visits to emergency departments, improve job prospects, and improve overall health outcomes.
The Issue
Medicaid is a key source of health care coverage for nearly 80 million people in the United States. While Medicaid provides comprehensive dental coverage for children, adult dental benefits are optional for states. As a result, coverage varies widely across the country, with many states offering limited or emergency-only care. This fragmented system leaves adults without the dental services they need. Impending cuts to Medicaid are expected to exacerbate the problem.
Why It Matters
Access to oral health care remains out of reach for many low-income families, with cost being one of the biggest barriers. Without stable, comprehensive dental benefits, people enrolled in Medicaid — particularly people with disabilities and residents of rural communities — are more vulnerable to preventable health issues. Lack of access to dental care can contribute to worse overall health outcomes and drive higher health care costs.
Dental coverage provides significant benefits for low-income adults. Regular oral health care can prevent dental issues from worsening and can contribute to improved overall health. It can even improve employment prospects: In a recent survey, nearly 18% of all adults reported that the appearance of their mouth and teeth affected their ability to interview for a job, with this figure rising to 29% among those with lower incomes. Insurance makes regular care possible and affordable.
Routine dental care can also reduce overall health care costs. Those without dental coverage often delay treatment until issues become severe or painful. This leads to visits to the emergency department (ED), which are significantly more expensive, costing an estimated $2.1 billion per year. Research from the American Dental Association (ADA) shows that nearly 79% of these visits could have been addressed in a dental office, which translates into potential savings of up to $1.7 billion per year.
The Impact of Medicaid Cuts
With recent federal legislation cutting Medicaid benefits, adult dental benefits are in danger. Experience, unfortunately, shows that these cuts will have devastating consequences.
In recent years, several states, including Oregon, Massachusetts, Maryland and Pennsylvania, cut Medicaid adult dental benefits (MADBs). As a result, low-income adults lost access to needed dental services, and their dental health suffered.
While these cuts are intended to reduce spending, experiences from those states show that eliminating or reducing MADBs often simply shifts costs from one part of the health care system to others. In many cases, when MADBs are cut, limited access to dental care leads more people to seek treatment in EDs, which are ill-equipped to meet oral health needs.
In both Oregon and California, initial “savings” derived from cuts to MADBs were quickly offset by increased ED costs and MADBs were ultimately restored in both states.
The experiences of these states show that reducing or eliminating MADBs is a short-sighted decision that harms patients, burdens health systems, and ultimately costs more in the long run.
The Path Forward
All adults enrolled in Medicaid should enjoy comprehensive oral health coverage, ensuring that low-income families can access timely and appropriate dental services.
By ensuring that states provide comprehensive dental benefits for adults who rely on Medicaid for their health coverage, policymakers can improve oral health outcomes, increase employment opportunities, and reduce long-term health care spending on chronic disease management and emergency department use.
Stats
80M
Nearly 80 million people rely on Medicaid for their health care.
Learn more
$2,918
Patients with diabetes would save approximately $2,918 annually if Medicaid covered periodontal care for adults.
Learn more
$2,437
The average dental ED visit costs on average $2,437, much higher than the average cost of a dental visit.
Learn more
21%
In Maryland, the elimination of Medicaid reimbursement for adult dental services led to a 21% increase in dental-related ED visits.
Learn more
60%
In Pennsylvania, spending on ED dental care has increased by more than 60% since the state cut MADBs in 2011.
Learn more
74%
More than 7 in 10 (74%) voters support adding adult dental benefits to Medicaid at the state or federal level.