 Early childhood caries remains the most common, preventable infectious disease among children in the United States.
Early childhood caries remains the most common, preventable infectious disease among children in the United States.
Preventing them is not always easy, though.
Many families, often those who are facing financial hardships or living in rural areas, struggle to connect their children to timely dental care. Barriers to access— including geographic location, language, cultural, and education — are a particular burden for families and children who would often benefit the most from the care.
But leaders in oral and primary care can and need to play an essential role in bridging gaps in access to care.
For example, dental providers can partner with schools to deliver dental care to underserved students. Medical teams and dental teams can work together to integrate oral health in pediatric primary care. These solutions, and others like them, can improve children’s dental access and advance equity, giving all kids a strong start.
Why Access to Children’s Dental Health Care Is Important
Major health organizations agree that dental care is especially crucial for babies. The American Dental Association, American Academy of Pediatrics, and American Academy of Pediatric Dentistry all advise that every child has a dental exam by the time they are 1 year old.
Despite this guidance and best intentions, many kids don’t have adequate dental care in their first few years. Recent CareQuest Institute research found:
- Most children enrolled in Medicaid don’t have their first dental exam until they are 3 years old.
- About 1 in 5 children with private insurance are 3–4 years old before their first oral exam.
In an August 2023 CareQuest Institute webinar, Francisco Ramos-Gomez, DDS, MS, MPH, director, UCLA Pediatric Dentistry Advanced Clinical Training Program, shared another glaring statistic: Among 4-year-olds today, nearly 7 in 10 children have dental disease.
When a child doesn’t get their first dental screening until their toddler years, they’re more likely to need restorative treatment, which is often more costly and invasive.
“The disease is so massive that you need to have a very specific specialist,” Ramos-Gomez explains, saying young children also need “all the things that require sedation . . . to really pursue treatment.”
Families and parents, of course, don’t foresee or want those situations. But a dental appointment can get skipped when inflexible occupations, transportation challenges, and priorities for other children in the family are added to the mix.
Emergency Departments Cannot Provide Adequate Dental Care
When a child experiences extreme pain from dental disease, families with limited access to dental care often turn to a hospital’s emergency department (ED).
This happens most frequently in Florida, where data were available, according to a 2023 CareQuest Institute analysis of nationwide ED visits by children under age 14 with non-traumatic dental conditions.
This study highlighted economic and racial disparities in Florida for such ED visits, which parallel national trends:
- More than 8 in 10 child ED visits for dental pain in Florida were for children enrolled in Medicaid.
- In Florida, children who were Black had more ED visits for dental symptoms than their peers of other racial groups.
However, EDs nationwide are ill-equipped to treat dental disease, whether for children or adults.
As Stacey Auger, a policy consultant at CareQuest Institute, describes in this video, while “folks leave the ED with a prescription for a pain medicine . . . the actual source of the trouble . . . is not met.”
Finding ways to improve access to dental care could prevent early childhood caries, reducing ED visits. Doing so would relieve already-strained health systems in communities and improve children’s well-being.
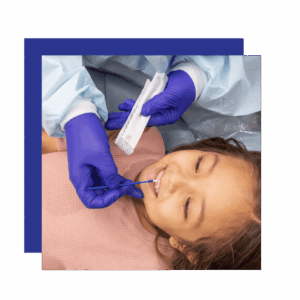
Fluoride varnish applied to child’s teeth
The Importance of Medical Well-Child Visits and Preventive Dental Visits
Primary care providers can have a critical impact on children’s dental health. CareQuest Institute research examining Medicaid claims data for children under age 4 found:
- Children who have a medical well-child visit are more likely to get preventive dental care.
- Compared to other children, however, 1-year-olds still have the fewest preventive dental visits.
Other recent analysis of more than 3 million Medicaid claims also found that medical-dental integration benefits children’s oral health:
- Most children covered by Medicaid get their well-child visit at an office and hospital, not a Federally Qualified Health Center (FQHC) or a rural or public health clinic.
- The study also validates that children are more likely to access preventive oral health care upon receiving this primary health care.
Medical-dental integration is clearly an effective approach to bolster child oral health.
Strategies to Improve Integration of Children’s Dental Care
Several solutions exist to increase equitable access to children’s oral health care. Here are three effective strategies that dental and medical providers can pursue.
1. Expand school-based dental sealant programs.
A 2023 CareQuest Institute webinar spotlighted school-based dental sealant programs. Sealants are proven to prevent dental disease in children. School-based programs broaden access to them, particularly for students without regular access to care.
The webinar offered success stories while highlighting a 2022 report on best practices for effective programs:
• Shailee Gupta, DDS, MPH, director of dental programs, St. David’s Foundation, notes her Texas program has reached more than 58,000 students since 1998.
• Helpful tips include assessing families’ needs, involving educators, and prioritizing schools where children are most at risk of tooth decay.
For Danica Loring, EFDA, CDA, dental practice director at Penobscot Community Health Care, school-based dental sealant programs have been a crucial place to begin rebuilding her center’s broader school-based dental program, which closed in 2020. It offers “an opportunity to see the kids’ oral health in general” to connect them to future care.
2. Embrace teledentistry as part of school services.
For dental care teams who cannot visit students in person, teledentistry is a worthy alternative. It is especially useful to reach rural children and other communities struggling with barriers to care.
One FQHC in North Carolina, Blue Ridge Health, partners with a school to run a teledentistry program. It helped more than 1,200 children access needed dental care in one year alone.
Teledentistry also promotes oral health equity. According to Stephanie Clester, RDH, MA, the clinical content and support specialist at CareQuest Institute, the technology enables dental teams to “reach more patients to reduce the burden of oral disease for those who need it most, making teledentistry a tool to achieve accessible and equitable oral health.”
3. Expand the use of oral health tools in primary care.
In July 2023, an American Medical Association new billing code took effect that advances medical-dental integration. It compensates medical providers for applying silver diamine fluoride (SDF), a liquid that gets brushed on to teeth to stop or prevent cavities.
As a non-invasive therapy, SDF can overcome barriers to dental care for children. It is especially promising for kids who see a medical provider but not a dental team. With this clinical tool in hand — plus new incentives to use it — primary care teams can do more to fight pediatric dental disease.
