Public understanding of the connection between oral health and overall health has steadily grown in recent years. There is also widespread and accumulating research that shows increasing dental coverage allows for more equitable access to dental care across communities, lowers overall health care spending on chronic disease management and emergency department usage, positively impacts oral health outcomes for patients, and increases employment opportunities. What’s more, the public is highly supportive of providing comprehensive dental benefits within Medicaid.
Fortunately, this research and the work of tireless oral health advocates are improving access to care for thousands of individuals in the United States.
The period between 2020 and 2022 marked a significant expansion of Medicaid adult benefits across the country — one of the most significant in recent decades. Nearly half of all states expanded their Medicaid adult dental benefit offerings, five states increased the amount of per member spending, and three states implemented benefits for the first time to some or all of their adult beneficiaries. In total, according to the just updated Medicaid Adult Dental Coverage Checker, eight states now offer an extensive Medicaid adult dental benefit.
And the momentum has continued into 2023, as new or expanded benefits have taken effect in five additional states: Hawaii, Maryland, Michigan, New Hampshire, and Tennessee. You can find more details about these changes on the Coverage Checker webpage. (Kentucky also enacted an expansion of Medicaid adult dental benefits via administrative regulation on January 1, but the benefits were rescinded on March 29.) Because the Coverage Checker shows benefits in place as of December 31, 2022, these benefits are not reflected on the updated dashboard.
Originally released in 2022, the Coverage Checker is an interactive tool for policymakers, administrators, and advocates to understand where a given state’s Medicaid adult dental benefits package falls on a continuum from no dental benefits to extensive benefits. It looks at coverage of specific procedures and services, including allowed frequency, in eight service categories. The Checker includes data self-reported by state Medicaid dental directors or their staff in a survey developed by the American Dental Association Health Policy Institute (ADA HPI), Center for Health Care Strategies (CHCS), National Academy for State Health Policy (NASHP), CareQuest Institute, and advisory committee members.
The updated Coverage Checker highlights the progress advocates and policymakers have made to expand adult dental benefits in the past few years. Here are the five most noteworthy takeaways:
1. The number of states that offer extensive Medicaid adult dental benefits has increased since 2020.
Although states are required to provide comprehensive dental benefits for children covered by Medicaid and the Children’s Health Insurance Program (CHIP), dental coverage for adult Medicaid beneficiaries is optional for states.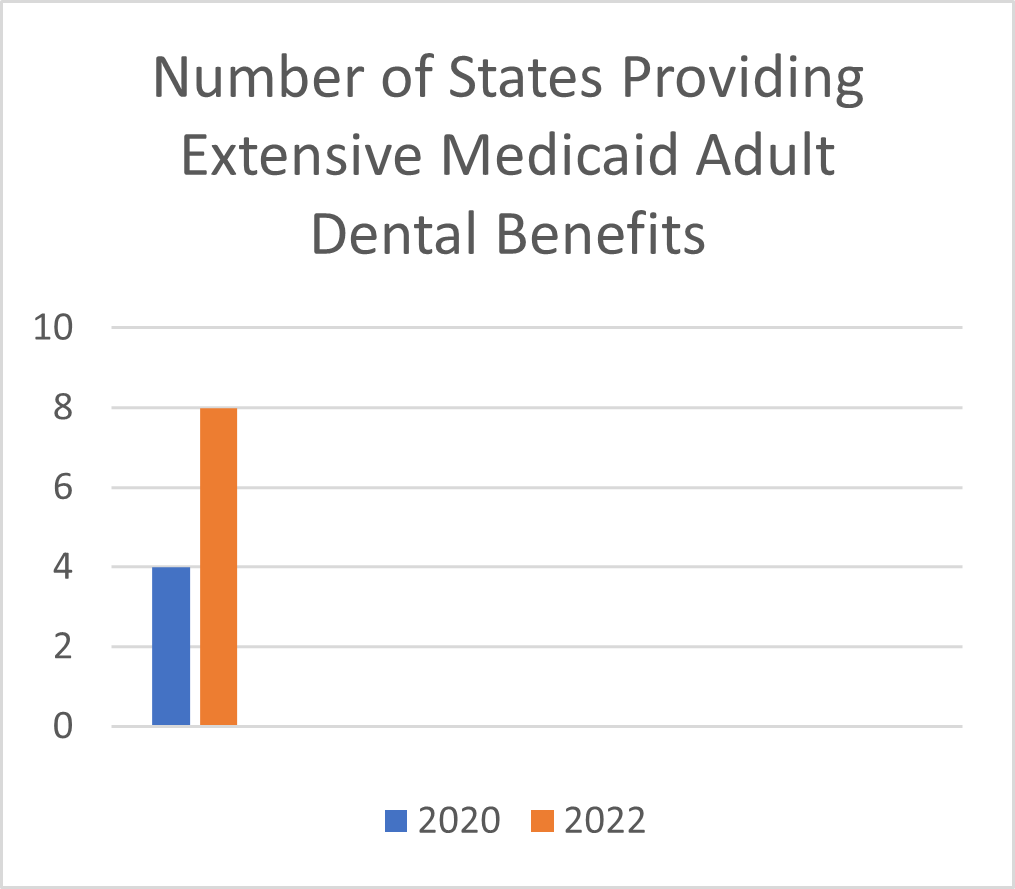
As a result, states have the option to limit the type or amount of services and beneficiary groups they will cover. States can also exclude adult dental services entirely.
In 2020, when data were collected for the original Coverage Checker, three states (Alaska, Nebraska, and Wisconsin) plus the District of Columbia provided an extensive dental benefit to the largest group of Categorically Needy Medicaid adult beneficiaries ages 21–64. (Categorically Needy is a term used by the Centers for Medicare and Medicaid Services.)
As of December 31, 2022, this number grew to the District of Columbia and seven states — Alaska, Iowa, Maine, Montana, New Jersey, Oregon, and Wisconsin — providing extensive dental benefits to the largest group of Categorically Needy Medicaid adult beneficiaries. (Note: Nebraska noted a reduction in their annual benefit maximum and coverage of partial dentures.)
2. Six states implemented adult dental benefits for the first time or significantly expanded their existing benefits.
Delaware, most notably, implemented a Medicaid dental benefit for all adult beneficiaries in October 2020. Prior to this, adult beneficiaries had no dental coverage in the state.
Five states — Kansas, Maine, Oklahoma, Virginia, and West Virginia — significantly expanded benefits to all adult members between 2020 and 2022. More specifically:
• In Kansas, Medicaid dental benefits were eliminated for all adults in 2010. (Between 2010 and 2022, Kansas provided emergency extractions to its adult Medicaid members. Some additional dental services were later offered through the state’s Managed Care Organizations as value-added benefits.) In 2013, the state’s three Medicaid-contracted managed care organizations (MCOs) began providing limited dental services to its adult members as “value-added services” at no cost to the state. They expanded those in 2018. In April 2022, the state budget was finalized and included funding for the restoration and expansion of Medicaid adult dental benefits. The new benefit (effective July 1, 2022) includes fillings, crowns, and periodontal treatment. The state’s MCOs continue to cover examinations and cleanings.
• In Maine, the state’s FY 2022 supplemental budget included funding to create an extensive Medicaid adult dental benefit. The benefit (effective July 1, 2022) provides coverage for diagnostic, preventive, restorative, endodontic, periodontal, prosthodontic, and adjunctive services as well as oral surgery. Prior to 2022, adult beneficiaries were covered only for emergency dental services.
• In Oklahoma, the state approved a Medicaid expansion ballot initiative in June 2020. As part of its implementation on July 1, 2021, the state also reinstated its Medicaid adult dental benefit. The benefit is available to all adult beneficiaries and includes preventive and restorative services, full and partial dentures, and extractions.
• In Virginia, in 2015, the state began providing an expansive dental benefit to pregnant adults. In 2019, the state enacted Medicaid Expansion, providing the state’s emergency-only Medicaid adult dental benefit to approximately 400,000 new enrollees. In November 2020, the state’s budget was finalized and included funding for an expanded Medicaid dental benefit for all adult beneficiaries, including diagnostic, preventive, restorative, endodontic, periodontal, prosthodontic, extraction, oral surgery, and adjunctive services.
• In West Virginia, in March 2020, the governor signed SB 648 into law, creating a limited Medicaid adult dental benefit. Coverage (effective January 1, 2021) is provided up to $1,000 per year and includes diagnostic, preventive, and restorative services.
3. Four states began providing an enhanced package of benefits to certain groups of adult beneficiaries.
Since the release of the original Coverage Checker, four states — Alabama, Louisiana, Maryland, Tennessee — began providing an enhanced benefits package to certain adult beneficiary groups between 2020 and 2022. Historically, Alabama, Maryland, and Tennessee have not provided dental benefits to their adult members. The expansion of benefits in these states marks a very significant change and, in Maryland and Tennessee, paved the way for an expansion of benefits to all adults in 2023.Of note, prior to January 1, 2023, Maryland Medicaid did not cover dental services for adults 21 years or older, except for pregnant and postpartum women, individuals enrolled in the Rare and Expensive Case Management, individuals enrolled in the Adult Dental Pilot Program, and emergency services for dental problems provided in a hospital emergency department.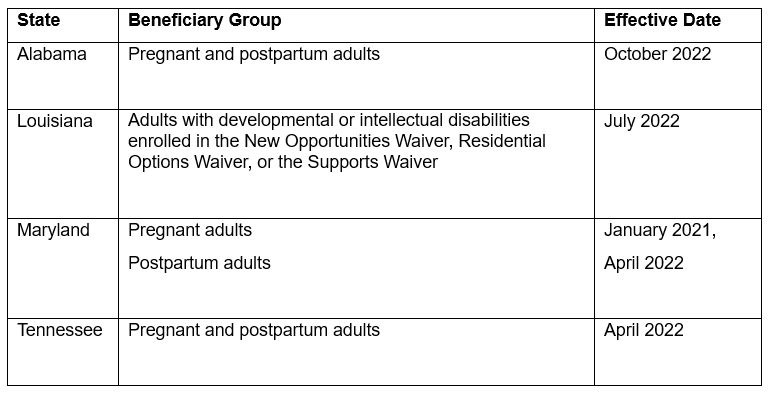
Beginning April 1, 2022, Maryland began providing dental benefits for postpartum women. Learn more about the Adult Dental Pilot Program in the state.
According to the survey that serves as the foundation for the Coverage Checker, 17 states reported that they offer different coverage — different amounts, durations, and scopes — to specific groups of beneficiaries than they offer to the largest group of Categorically Needy Medicaid adults ages 21–64. Within those states, the beneficiary groups most commonly covered are pregnant and postpartum adults, adults with developmental and/or intellectual disabilities, and adults utilizing long-term care.
Additionally, some states offer coverage to adults with blindness (Missouri and Utah), those experiencing homelessness and/or substance use disorder or mental health conditions (Utah), former foster youth (Maryland), and adults who are dually eligible for Medicaid and Medicare (Maryland). Later this year, CareQuest Institute plans to publish a separate report detailing those groups of adult beneficiaries.
4. Nearly 40% of states have expanded benefits since 2020.
Twenty states expanded their benefits between 2020 and 2022.
Four added at least one service (e.g., cleaning, periodontal services, or complete dentures), twelve added between two and six services, and four states added seven or more services.
The most commonly added services were:
- Complete dentures
- Chairside or laboratory reline of complete dentures, and rebase
- Periodontal scaling and root planing, and periodontal maintenance
- Resin-based partial dentures
- Amalgam and resin-based composite restorations
- Prophylaxis
5. Sixty-two percent of states have no annual limit on dental services spending per member.
Thirty-two states place no limit on dental services spending per member per year. Four states have an annual benefit limit of less than $1,000, and another four have an annual benefit limit of $1,000 or greater.

Stacey Auger, MPH
Between 2020 and 2022, five states (Iowa, Oklahoma, Kansas, South Dakota, and Vermont) increased their annual benefit maximum.
Authored by Stacey Auger, MPH, policy consultant, CareQuest Institute
Editor’s note: Explore the full Adult Dental Medicaid Coverage Checker and state-by-state details in the interactive dashboard. There, you can also learn more about the survey that assesses the effectiveness of
